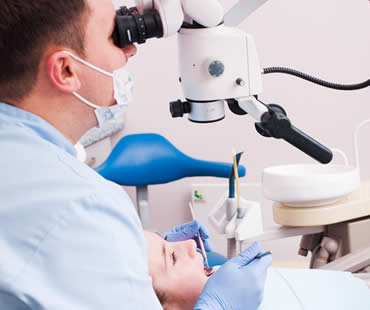
Your family, general, or pediatric dentist or orthodontist may refer you to an oral and maxillofacial surgeon for some dental treatments that require oral surgery. An oral surgeon is a specialist who has graduated from an accredited dental school and also completed additional education and residency related to surgical procedures needed to treat various oral diseases and conditions. An oral surgeon is trained in treating the following conditions:
- Removal of diseased or impacted teeth
- Placement of dental implants
- Treatment of facial trauma involving gums, jaws, nasal cavities, cheekbones, eye sockets, and forehead
- Evaluation of pathologic conditions such as cysts and tumors of the mouth and face or acute infections of the oral cavity, salivary glands, neck, and jaws
- Treatment of facial pain including those caused by temporomandibular (TMJ) problems
- Cosmetic or reconstructive surgery to correct jaw, facial bone, and facial soft tissue problems
- Corrective jaw surgery
- Cleft lip and cleft palate repair
- Surgical treatment for sleep apnea
There are many different techniques that oral surgeons use to accomplish your treatment goals. The choice of techniques may vary between surgeons and should be discussed between you and your surgeon prior to the procedure.
Many oral surgery procedures can be completed in an outpatient setting. Often you are only in the office for a few hours and can return to your regular routine in a matter of days. A good oral surgeon will be able to perform these procedures with little chance of complications, and will be able to provide you with the information you need to understand the recovery process. Your oral surgeon will often collaborate with other specialists, such as an orthodontist or cosmetic dentist, to achieve your ultimate treatment goals.
If you live in the Baltimore area contact us today
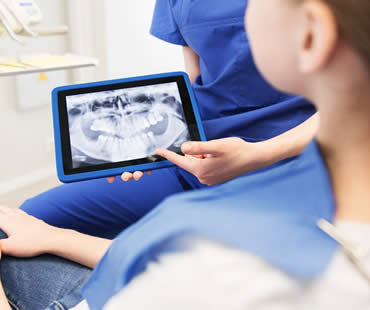
Wisdom teeth are the third set of molars and the last adult teeth to erupt into the mouth. Most people have four wisdom teeth, two on the bottom and two on top. Many people do not have enough room for these molars to emerge completely, causing them to become impacted in the gum. Impacted wisdom teeth are difficult to clean, making them more susceptible to decay and disease. Other dental problems caused by impacted wisdom teeth include pain, damage to surrounding teeth, and bite alignment issues. For these reasons, your dentist may recommend having the impacted teeth removed to prevent future problems.
Surgery to extract an impacted wisdom tooth or set of wisdom teeth is usually an outpatient procedure done in your dentist or oral surgeon’s office. If the tooth or surrounding area are deemed to have an infection prior to the procedure, surgery will be delayed, and your dental professional will likely prescribe antibiotics to help heal the area.
On the day of surgery, local anesthesia will be administered to numb the area where the extracted tooth will be removed. Depending on the severity of your case, your dentist or oral surgeon may also utilize a general anesthetic.
Once the anesthesia has taken effect, an incision will be made to open up the gum and any bone blocking the tooth will be removed. Your dentist or surgeon will then separate the tissue connecting the bone to the tooth and extract the tooth. Some teeth are too large to remove in one piece, in which case your surgeon will cut the tooth into smaller pieces to make it easier to remove. Finally, the incision is closed with stitches and packed with gauze to help alleviate bleeding.
Long-term complications from impacted wisdom tooth surgery are rare. To ensure a successful recovery from this or any oral surgery, be sure to follow all aftercare instructions provided by your dentist or oral surgeon.
We treat patients from Baltimore and the surrounding area
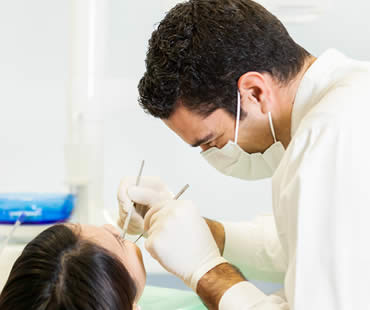
Wisdom teeth are the last adult teeth to erupt into the mouth, generally emerging between the ages of seventeen and twenty-one. They are the third set of molars and are in pairs: two each on the top and bottom arch of teeth. While some patients don’t have wisdom teeth, most do. Many of those who do have them don’t have enough room for those teeth to erupt fully, causing them to be wedged under the back of another tooth, impacted in the gum.
Impacted wisdom teeth are very difficult to clean, and can negatively affect the surrounding teeth. They are highly vulnerable to disease and decay and may lead to tooth pain and damage to adjacent teeth. For these and other reasons, a dentist may recommend that the teeth be extracted through oral surgery as soon as necessary to prevent any problems.
Extraction of wisdom teeth is typically an outpatient procedure done in an oral surgeon’s office. A healthy patient can proceed with a typical surgery, but if any infection is detected, the surgery can’t move forward until the infection is cleared up through the use of a full course of antibiotics. Once the surgery is moving forward, the surgeon’s team will administer some form of anesthesia to numb the area surrounding the tooth or to possibly sedate the patient through IV sedation dentistry.
After the anesthesia has fully taken effect, the surgeon makes an incision to open the gum and to remove any bone that is blocking the tooth from extraction. The tissue connecting the bone to the tooth will be separated and the tooth will be removed. In some cases, the surgeon will have to break the tooth into smaller pieces to make it easier to remove. After thoroughly cleaning the area and removing any remaining debris, the incision will be closed, stitched and packed with sterile cotton gauze to staunch any bleeding.
The surgeon will provide aftercare instructions. Patients should follow these instructions to the letter in order to ensure the best and fastest healing of the surgical site.
We treat patients from Baltimore and the surrounding area
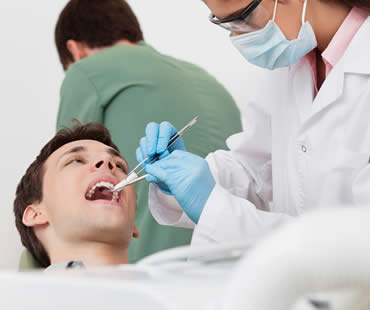
There are a number of reasons that dentists or oral surgeons recommend surgery, but facial injuries are probably the most unexpected and alarming cause. Maxillofacial injury, or facial trauma, refers to any injury to the mouth, jaw, and face. Most of these injuries result from sports, car accidents, job accidents, violence, or an accident at home. Let’s learn about oral surgery resulting from facial trauma.
Broken bones are a common type of serious facial injury. Fractures can occur in the upper or lower jaw, cheekbones, palate, and eye sockets. Injuries in these locations may affect vision and the ability to eat, talk, and breathe. Hospitalization is often required for treatment, which is similar to that for fractures in other parts of the body. The bones must be lined up and held in place to allow time to heal them in the correct position. Because casts are not possible in facial injuries, the surgeon may use wires, screws, or plates to treat fractures. Sometimes healing takes as long as six weeks or more.
Even though some facial injuries are worse than others, all of them should be taken seriously. They affect an important area of the body, so it is recommended to seek treatment from an oral surgeon to make sure you receive optimum care. Even if stitches are all that’s required, it’s best to have them performed by an oral surgeon who can place them exactly as needed to produce the best results.
It’s no surprise that the best solution for facial injuries is to prevent them in the first place. Oral surgeons suggest consistent use of mouth guards, seat belts, and masks and helmets as required. Improvements have been made to safety gear to make these items more comfortable and efficient, so there should be no excuses for not using them to protect yourself and avoid injuries that can lead to oral surgery.
Our dental office is located in Baltimore

Obstructive sleep apnea is a condition created when a portion of the upper airway is blocked, causing breathing interruptions during sleep and low blood oxygen levels. As many as 20% of adults are affected by mild obstructive sleep apnea, while one in fifteen suffers from more severe apnea.
Symptoms of obstructive sleep apnea include snoring, extreme daytime drowsiness, restless sleep, high blood pressure, depression, problems with mental function, as well as a host of other mental and physical concerns. Left untreated, obstructive sleep apnea can lead to a long list of serious medical conditions, including hypertension, heart attack and stroke.
If you have been diagnosed with obstructive sleep apnea, your doctor may initially treat the condition with a CPAP device that you wear while sleeping. While a CPAP machine will reduce the obstruction to the airway, it is not a cure and will only be effective during use. Other non-surgical treatment recommendations may include the wearing of mouthguards to reposition the jaw, sleep position changes, or weight loss.
Tongue muscle advancement involves moving the bony attachment of the tongue muscles, and can be combined with palatal surgery to reduce excess tissues. This therapy may also include removing enlarged tonsils and nasal surgery. These treatments are most often used for milder cases of obstructive sleep apnea.
However, if these treatments do not work or for more severe cases of obstructive sleep apnea, oral surgery offers solutions to correct apnea. Maxillomandibular Advancement is a procedure that repositions the upper and lower jaw and chin to open the airway. This treatment is highly successful and offers the greatest chance of permanent correction in moderate to severe cases of obstructive sleep apnea.
For more information about how surgical therapies and treatments can be utilized to address your obstructive sleep apnea, consult with a qualified oral and maxillofacial surgeon.
Schedule your appointment at our Baltimore dental office

While minor gum recession can be treated by your dentist with deep cleaning and antibiotics, serious gum recession can only be treated with oral surgery. A loss of bone and gum pockets that are very deep require gum surgery to address the pain and damage left by acute gum recession.
Three treatments are used primarily in the treatment of serious gum recession, in order of invasiveness: pocket depth reduction, regeneration, and soft tissue graft. Pocket depth reduction involves a deep cleaning of the affected area. The periodontist folds the gum tissue back and utilizes tooth scaling and root planing to remove any tartar and plaque built up around the tooth. Once the gum pockets are clean, the surgeon pulls the gum tissue gently around the tooth, eliminating the deep pockets altogether or significantly reducing their depth.
Regeneration utilizes a similar treatment to pocket depth reduction, but it also addresses any bone loss that occurred due to acute gum recession. In this process, a regenerative agent such as graft tissue, membranes or tissue stimulating proteins is added to the affected area. The gum tissue is then tucked into place and stitched down. Over time, the regenerative agent will work to rebuild lost bone and tissue, leaving healthy and thriving tissue behind.
The most common soft tissue graft is taken from the patient’s own mouth, either by removing tissue from the roof of the mouth or from the gum tissue near the affected tooth. The healthy gum tissue is placed in the affected area, over the exposed tooth root, protecting it from infection and damage.
To prevent the need for oral surgery to address your receding gums, have good oral hygiene habits. Brush, floss and see your dentist twice a year for checkups and professional cleanings. Talk to your dentist if you have any other questions about how to reverse or prevent gum recession.
If you live in the Baltimore area contact us today