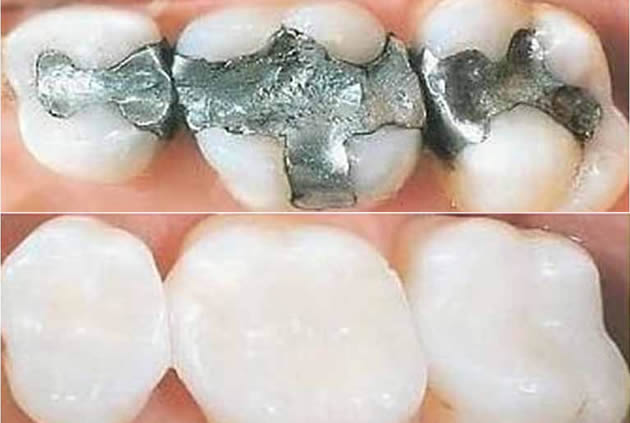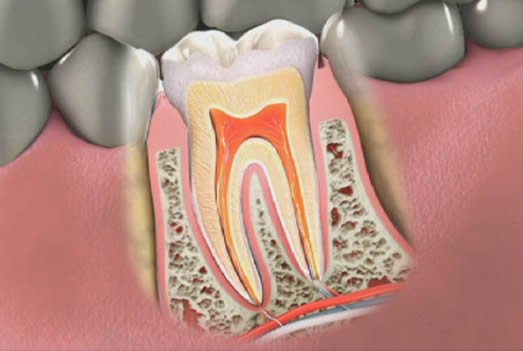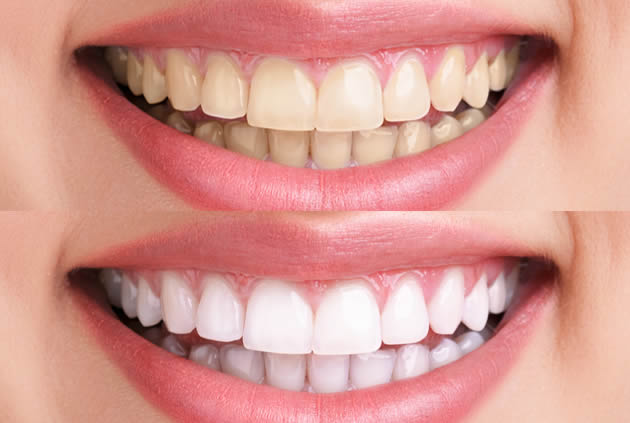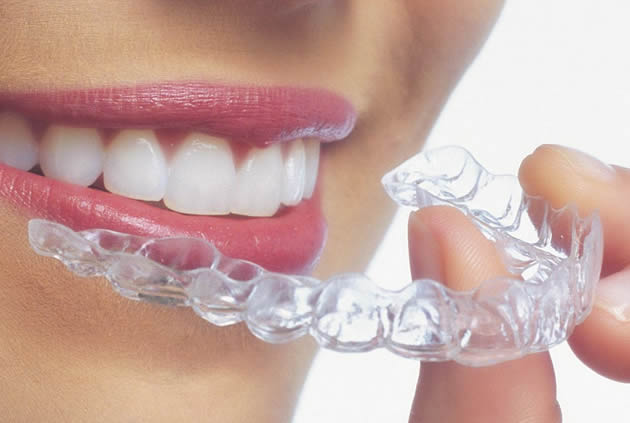
Gum disease is a serious problem. You should treat it as soon as possible following the recommendations of your dentist. Also known as periodontal disease, it has several treatments, depending on the severity of the issue.
Your first course of action is to completely revamp your oral hygiene habits. Daily flossing and brushing following meals are essential habits to develop. You must have a clean mouth before you go to bed. If you smoke, you should stop. Your mouth’s health depends on it.
If you haven’t been keeping up with your professional checkups and cleanings, you need to start again. Long-term gum health is greatly impacted by the plaque, tartar, food debris and bacteria left on teeth. Hardened calculus, or calcified plaque, can be removed using a process called scaling. This process may require local anesthesia.
Your progress will be evaluated by your dentist to see if your gum tissue is recovering. With enough progress and response to treatment, your gum disease treatment may not progress beyond these initial steps; however, for more severe cases of gum disease, you may require oral surgery.
Surgical procedures are available that can regenerate and repair the soft gum tissue in the mouth, as well as hard tissues such as bone or teeth. Your oral surgeon will want to reduce or completely eliminate gum pockets, or open areas beneath the gum line, improving and renewing gum to tooth attachment. Normal oral functions and aesthetic appearances are aimed to be restored.
There are many sedation dentistry options available to patients treating their gum disease with oral surgery. These include local anesthesia and IV or conscious oral sedation. Talk to your oral surgeon to see what’s appropriate for your specific needs.
Don’t wait to treat your gum disease. Do what you need to do to ensure a lifetime of better oral hygiene and gum health.
We treat patients from Baltimore and the surrounding area

If oral surgery is in your future, you might be worried about what’s to come. The way to relieve that worry is to talk to your oral surgeon. Your oral surgeon has the experience and knowledge necessary to guide you through whatever concerns or questions you may have. Here is a guide to some of those questions and answers:
How will I handle pain following surgery?
- In many cases, you will have been prescribed narcotic pain relievers. If you are taking narcotics, take them only as recommended and do not mix them with over-the-counter pain relievers or alcohol. Driving while on narcotics is dangerous and can have serious consequences for you personally and for others. If you weren’t prescribed any medication, use anti-inflammatory analgesics such as ibuprofen or naproxen sodium.
What will happen to my stitches in the days following surgery?
- Some stitches will be designed to dissolve over time and will not need to be removed. Others will not come out on their own and will need to be removed at a subsequent appointment. In many cases, losing a single stitch or two in the days following surgery isn’t serious; however, for bone-graft treatments, it is problematic and you should contact your surgeon immediately.
Can I eat normally after surgery?
- Immediately after surgery when you’re still experiencing any mouth or tongue numbness, don’t eat anything. You could mistake the soft tissues of your mouth for food and do serious damage to your mouth without realizing it. After your numbness subsides, consume soft foods of tepid temperatures for several days to allow for healing. Talk to your surgeon to learn when you can resume normal eating patterns as dictated by your particular surgery.
What other tips do you have?
- Stay hydrated and rest as much as possible to facilitate complete and quick healing. Call your surgeon if you have excessive bleeding or pain that doesn’t lessen with time. Be aware of signs of infection (swelling, redness, odorous or sour discharge) at the surgical site and seek professional care when needed.
We look forward to seeing you in our Baltimore dental office
Oral surgery to correct problems with the jaw is known as orthognathic surgery. Jaw issues can result from birth defects, changes due to growth, or injury or trauma to the face. While orthodontics can correct bite problems when only the teeth are involved, oral surgery may be required when repositioning of the jaw is necessary to correct the issue. If you suffer from any of the following concerns, orthognathic surgery may be a consideration:
- Difficulty chewing, biting or swallowing
- Problems with opening and closing your mouth, or with speaking
- Persistent jaw or temporomandibular joint pain
- Clenching or grinding of teeth causing excessive wear to the teeth
- Inability to make the lips meet without straining
- Un-proportional facial appearance or protruding jaw
- Malocclusion, open, or incorrect bite
- Recessive lower jaw and chin
- Sleep apnea and breathing problems
Most jaw surgeries are performed completely in the mouth, so no facial scars are visible. The oral surgeon makes cuts in the jawbone and then moves them to the correct position. Once the jaw is correctly aligned, screws and bone plates are placed to secure the jaw into the new position. Sometimes it may be necessary to add extra bone to the jaw from your hip, leg, or rib.
Orthognathic surgery is performed by an oral and maxillofacial surgeon usually in a hospital setting. Recovery time from jaw surgery takes three to six weeks. Your general or family dentist should be able to refer you to a skilled oral surgeon for a consultation and examination to determine a treatment plan. Jaw surgery can improve not only your facial appearance, but also chewing, speaking and breathing functions.
Schedule your appointment at our Baltimore dental office

If you or a loved one is scheduled to have or has recently had oral surgery, you probably have a lot of questions. Here are some of the most common questions:
- One of my stitches came out after my surgery, should I be worried? Losing a stitch isn’t a problem. In the majority of cases, stitches are put in place during surgery to assist in clot formation and bleeding control. If you have undergone a bone-graft procedure, however, contact your surgeon because you may need to be seen immediately.
- What can I eat after surgery? Immediately following surgery, eat only soft foods of tepid temperature. Avoid very hot or very cold foods. Eat nothing that is crunchy or chewy so you won’t damage the surgical site.
- I am having a lot of pain following my procedure, what should I do? If you have been prescribed pain medication, take it as recommended. If no prescription was given, use over-the-counter medicines containing natural anti-inflammatory properties such as ibuprofen. Stay hydrated by drinking room temperature water and get plenty of rest.
- I had a tooth extracted, how can I tell if I have a dry socket? Dry socket is the result of the loss of the blood clot present in the extraction site. Smoking, using a straw, poor oral hygiene or failure to rest properly following the extraction procedure can lead to this condition. Typically dry socket will present within one week of extraction and is treated with sterile wash and pain-relieving, medicated gauze.
- I had a procedure this morning and am still bleeding. Is that normal? Bleeding following extractions or other surgical procedures is common. If you are bleeding more than normal, bite down on some sterile gauze or a damp teabag for twenty or thirty minutes. Don’t keep removing the gauze to look for blood; that can make the bleeding worse. Call your surgeon if you feel your bleeding is excessive.
Your oral surgeon can answer these questions and more. Don’t hesitate to call the surgeon’s office to get the peace of mind you require to heal comfortably following your procedure.
Our dental office is located in Baltimore
Wisdom teeth, your third set of molars, are named that because they are the final teeth to erupt. They usually come in between ages 17 to 25, and are located in the very back of your mouth on the top and bottom. Your dentist will examine you to find out if your wisdom teeth are properly positioned and healthy. If they aren’t, your dentist will recommend removal.
How do you know wisdom teeth should be removed?
Some of the signs there is a problem with your wisdom teeth include pain, infection, cysts, gum disease, damage to nearby teeth, and tooth decay. If you experience any of these symptoms, see your dentist for an examination.
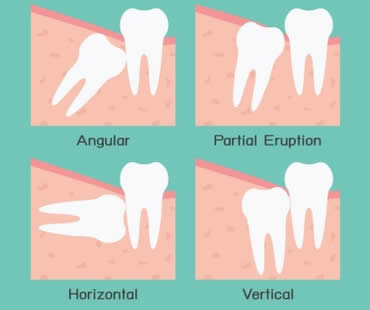
What are impacted wisdom teeth?
Sometimes your teeth just don’t have room to grow in properly. They can erupt at angles within your jaw, sometimes even horizontally. If wisdom teeth aren’t able to erupt normally they can become trapped, or impacted, inside your jaw. Symptoms of impacted wisdom teeth are pain, infection, and swelling. When teeth are impacted, they can lead to serious problems. Many dentists want to avoid impacted teeth and therefore remove your wisdom teeth before they erupt or grow too big.
Are there less obvious reasons to remove wisdom teeth?
It’s not always clear when these teeth way in the back of your mouth are causing problems, or might in the future. Many dentists remove them in teens or young adults so they don’t cause problems later, or become too firmly planted in the jaw. Also, sometimes wisdom teeth are removed as part of orthodontic, periodontal, or restorative treatment plans.
What happens if I don’t have them removed?
Some dentists prefer to wait and see what happens with time to your wisdom teeth. Make sure you continue to have these teeth monitored, because the risk of problems doesn’t go away with age. Removing wisdom teeth isn’t always necessary, because if there’s room in your mouth and they come in properly, they work just like any other teeth. The key is to watch them to make sure problems don’t arise in the future.
Dental office for wisdom teeth removal
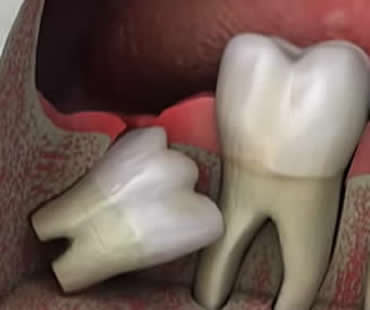
Also called third molars, wisdom teeth are the last set of teeth to erupt. Usually, people get their wisdom teeth in during their late teens and early 20s. Although some individuals have no trouble with their wisdom teeth, many people end up having these teeth removed because they may become impacted and create dental health issues. Learn more about wisdom teeth with this Q and A:
Do I need to have my wisdom teeth removed?
If your wisdom teeth aren’t causing problems, you can leave them alone. Typically, wisdom teeth are crooked or impacted, which can generate problems with the surrounding teeth. Also, wisdom teeth can be harder to keep clean, so the risk of decay on these teeth is higher.
When should I have these teeth taken out?
For optimal results, most dentists recommend wisdom teeth removal for patients when they are between 16 and 22 years old. The formation of the roots isn’t complete, so you have fewer complications.
Are there any risks?
As with any surgery, you can have issues arise, but the biggest concerns are nerve damage and dry sockets. Older patients have a greater chance of nerve damage because the root has more fully developed. Dry sockets occur when the post-surgery blood clots dislodge.
Does my age matter?
Some adults don’t experience any symptoms until they are in their 30s, 40s, or 50s. You can have these teeth extracted at any point, but when you get older, surgery is more difficult and the recovery takes longer. If you have trouble with your wisdom teeth, contact your dentist right away for a complete exam.
Baltimore dental office for wisdom teeth – White Marsh Family Dentistry